Blog
Mar 16, 2026
Home Health Nurse Scheduling Is Broken

Laurel Chiaramonte

Let me tell you about how a spreadsheet tried to ruin my life.
It was taped to the door of the nurses' station about a month before the schedule was supposed to go out. I would ask everyone to fill in the days they could not work. Two weeks later, I would pull it down and disappear into my office for a weekend of schedule writing.
Sometimes it took 12 hours. Sometimes 18. Often, more than that.
I was a charge nurse on a small military floor, maybe 40 nurses total. I would sit there manually trying to account for who needed weekends off, who was certified to be charge nurse, who was already carrying extra shifts, and who had a conflict I remembered from a conversation two weeks earlier. I would come up with one or two possible configurations and pick the least bad option. Then I would tape the schedule to the door and wait for the complaints.
… and there were always complaints.
My husband watched this process a few times. He was working on his PhD in industrial engineering. He looked at what I was doing and said: This could be fixed with algorithms.

I did not fully understand what that meant at the time. What I understood was that I was exhausted, my nurses were unhappy with any schedule I produced, and some of them genuinely believed I was playing favorites. I was not. I was just trying to get through it.
He spent months researching the problem. What he found was that even for my small floor, there were over 7,000 variables in play when I wrote that schedule. My brain could realistically hold a few alternative schedule configurations at a time. His algorithm looked at tens of thousands of potential schedules and returned the best one in under five minutes.
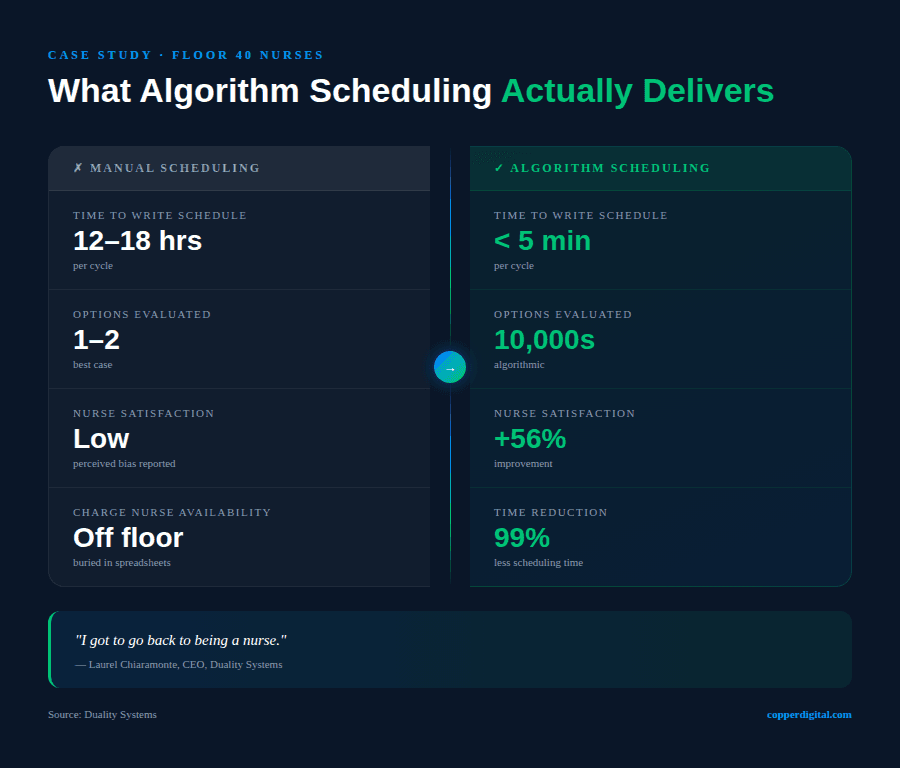
The results were measurable and shocking. Scheduling time dropped by more than 99 percent. Nurse satisfaction with the schedule improved by 56 percent. And the perception of bias disappeared, because you can’t accuse a computer of having favorites.
More than anything else, I got to go back to being a nurse and a leader.
The part nobody talks about
There is a version of this story where we immediately built a company, took it to market, and hospitals lined up to buy it. That is not what happened.
We went to the market in 2021. COVID had just happened. Hospital budgets were wrecked. And we ran into something I have since heard from many other health-tech founders: the people who feel the pain are very rarely the people who hold the budget.
I knew exactly how much that scheduling problem cost me. I could feel it in the hours I was not being a nurse, in the patients I was not with, in the nurses I was not leading because I was buried in a spreadsheet. But the person three rungs above me looked at the situation and saw a problem that was, technically, getting solved. The schedule got made. Why pay for something else to do it?
They did not see the ground floor. They rarely do.
This is not a Duality Systems problem specifically. A 2025 study in JMIR Formative Research found that nurses consistently report scheduling practices as a driver of burnout and turnover, and that management rarely has visibility into the day-to-day experience of unfair or inflexible schedules. The research gap between what nurses experience and what leadership measures is real.
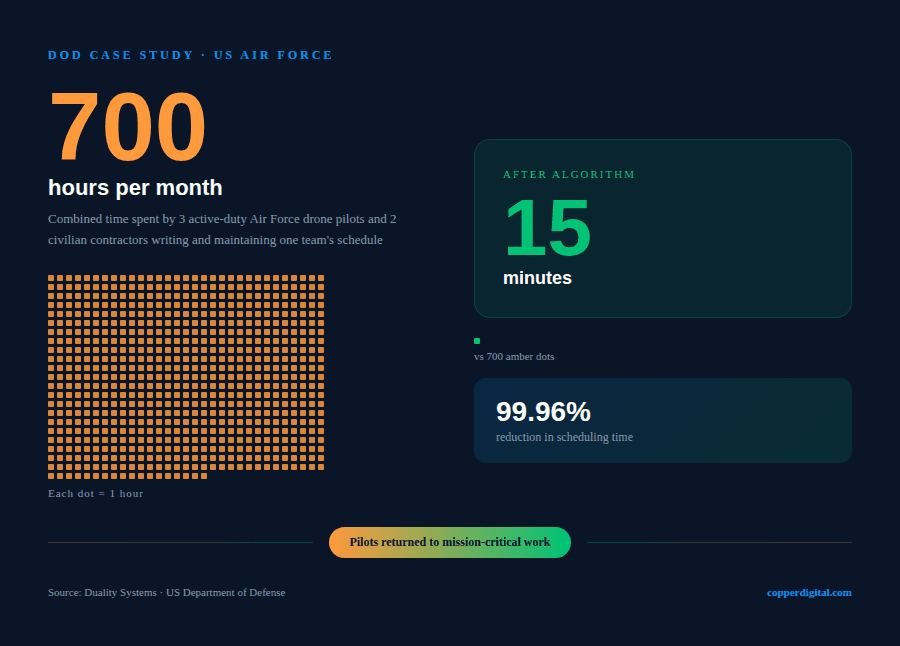
So we pivoted. We are a veteran-owned small business, about 85 percent veterans on a team of eight. We went to the Department of Defense and found that the scheduling problem looks almost identical, no matter the setting. Drone pilots. Satellite watch floors. Missile silo operations. Different certifications, different stakes, same structure: thousands of variables, 24-hour coverage requirements, billions of possible configurations that a human brain cannot fully evaluate.
We took a team of Air Force drone pilots and civilian contractors, spending 700 combined hours a month writing and maintaining a schedule. We got that to 15 minutes. The technology works. That has never been the question.
Why home health scheduling is a harder version of the same problem
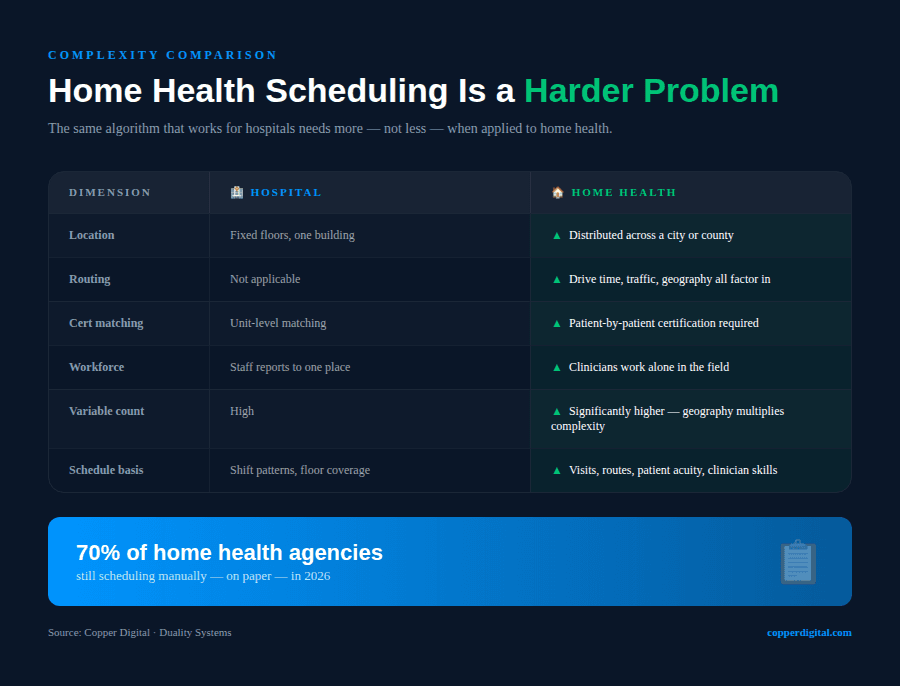
When I talked with Arvind Sarin of Copper Digital recently, something he said stopped me. He mentioned that among the dozens of home health agencies he speaks with every month, roughly 70 percent still schedule manually. On paper. In 2026.
Home health scheduling is actually a harder problem than hospital scheduling. In a hospital, you are assigning nurses to floors. In home health, you are routing clinicians across a geography, matching certifications to patient needs, accounting for drive time, and doing it all for a workforce already stretched thin.
The math is not forgiving. The number of possible schedule configurations grows factorially as you add staff and patients. A scheduler managing 15 nurses across a metro area is working with a problem space that is, effectively, impossible to optimize by hand. They are making the best choice they can see, not the best choice that exists. The U.S. AI nurse scheduling software market was valued at $55 million in 2024 and is projected to reach $516 million by 2033, largely because manual methods are finally being recognised as structurally insufficient, not just inconvenient.
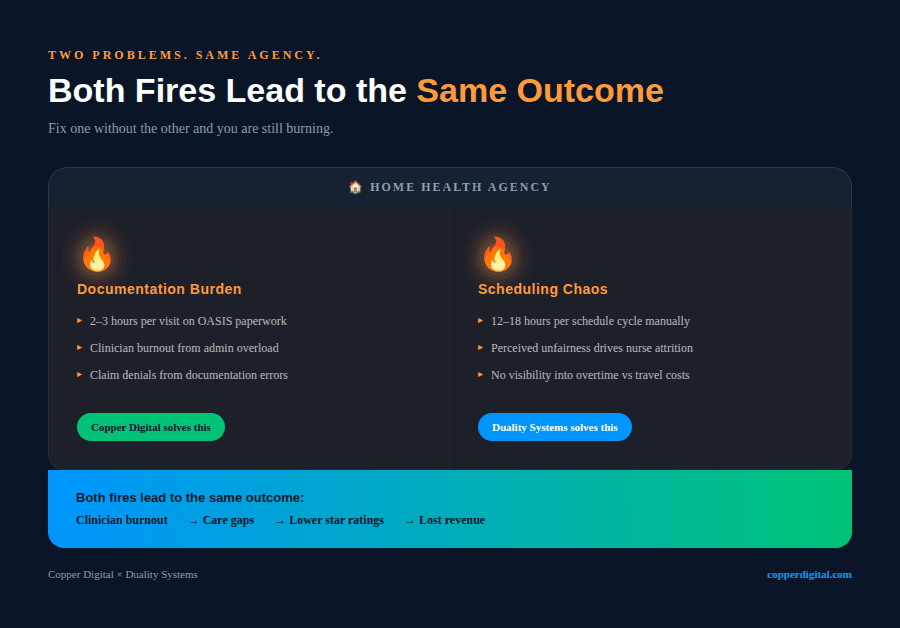
Copper Digital focuses on the documentation side of this problem. OASIS documentation automation is their Act 1, and it is the right call. If a clinician is spending two to three hours on paperwork after every visit, that is the first fire to put out. But scheduling is the fire in the next room. Both are burning.
What makes people resistant, and why that is changing
When people hear that we use AI, the conversation often goes sideways.
Most people think AI means a large language model. They think of something that takes a prompt and generates text. Our AI is not that. It is combinatorial optimization: algorithms that evaluate possible schedule configurations at a scale no human can match. It is not going to write your emails or summarize your meeting notes.
But in an environment where the word AI triggers either excitement or fear, that distinction is hard to communicate quickly. Add HIPAA concerns, security concerns, change fatigue inside large healthcare organizations, and the reality of being eight people trying to get a meeting with a hospital system, and you start to understand why selling into healthcare is harder than it looks from the outside.
There is also a structural procurement problem. Home health agencies, even mid-sized ones, often run intake, scheduling, and documentation workflows on separate, disconnected systems. Each one requires a separate buying decision, a separate champion inside the organization, and a separate implementation. The agencies that struggle most are often the ones trying to solve every problem at once or none at all.
If it is taking you more than an hour to write a schedule, you are spending that time somewhere you could be spending it better.
I still believe healthcare is where this belongs. My whole career as a clinical nurse specialist has been oriented around one thing: improving the efficiency and effectiveness of healthcare delivery. Not in the abstract. In the practical, ground-level sense, nurses cannot take care of patients when they themselves are not okay.
And a lot of what makes nurses not okay is fixable with the schedule.
The 85-to-90 percent solution
I learned something that changed how I thought about what we were building.
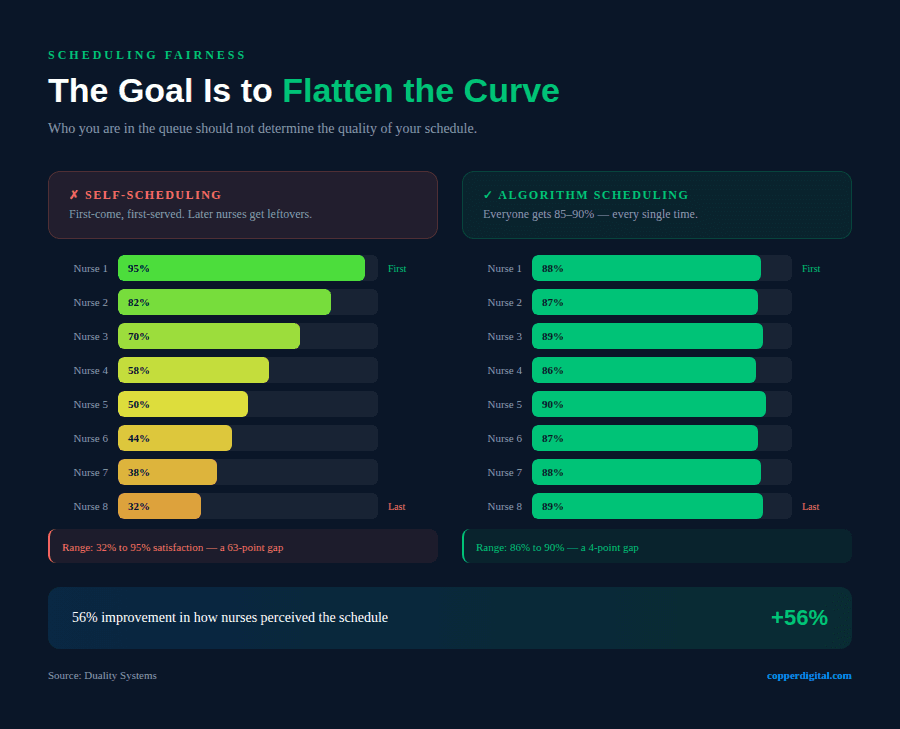
Self-scheduling sounds like it gives nurses control. In practice, it creates a different problem. If you are the first person to self-schedule, you get a good pattern. If you are last, you get whatever is left. So some nurses end up with schedules they can live with, and some feel like they are always at the bottom of the pile. The inequality is real, and people feel it.
What I wanted was to flatten that curve. Not to give everyone a perfect schedule is not possible. But to give everyone an 85-to-90 percent solution, every single time.
That means if I prefer to work weekends, that preference goes into the algorithm as a variable. If I need a specific pattern for a family situation, that goes in, too. The algorithm does not just minimize conflicts; it maximizes fairness across the whole group, transparently, so when a nurse looks at the schedule and wonders why she got that shift, there is an answer that has nothing to do with whether the charge nurse likes her.
We are also developing a shift bidding system. When a shift opens up, instead of defaulting to overtime or a travel nurse, you can open it internally first. Leadership sees in real time what filling the shift internally would cost versus externally, and can make that call with data. Unplanned overtime and travel nurse costs are among the top margin pressures for home health agencies right now. Having a system that makes those tradeoffs visible before the decision is made changes the math entirely.
A word about human oversight
I want to be direct about something, because I think the AI conversation in healthcare tends to land in one of two wrong places: dismiss it entirely, or hand it the wheel completely.
We always want a human to review the output. The algorithm produces a schedule that a person then looks at and says: Yes, this makes sense, or, We need to adjust this one. That review step is not a failure of the technology. It is the point.
You have to know what right looks like before you can evaluate what the algorithm gives you. If you skip that step because the output looks plausible, you are not using AI as a tool. You are outsourcing your judgment to a machine and hoping for the best.
This is consistent with where the research is landing, too. The JMIR study cited earlier concluded that a hybrid approach integrating AI recommendations with human decision-making is optimal for nurse scheduling, not full automation, not manual scheduling with a software veneer, but a genuine collaboration between algorithm and human judgment.
Copper Digital takes the same approach with documentation. Their system does not replace the clinician's clinical judgment; it handles the structural work so the clinician can focus on the actual assessment. The difference between brittle automation and intelligent automation is whether there is a guardrail, and that distinction matters enormously in healthcare, where the cost of a wrong output is not just an inconvenience.
What this means for home health agencies right now
The nursing shortage is not going away. According to the American Nurses Association, the U.S. is projected to need more than 200,000 new nurses per year through 2026 to meet demand. Home health is competing for those nurses against hospitals, SNFs, and outpatient clinics and losing, largely because the job is harder and the support infrastructure is thinner.
You cannot out-recruit a structural problem. You can only make the job worth staying in. That means better pay where possible, yes. But it also means schedules that respect people's time, intake processes that do not dump unnecessary administrative work on clinicians, and documentation systems that do not require two hours of paperwork after every visit.
The agencies that figure this out first will have a retention advantage that compounds over time. The ones that keep treating scheduling, documentation, and intake as separate manual problems will keep paying for travel nurses, keep losing their best clinicians to less chaotic environments, and keep wondering why their referral sources are calling someone else.
Copper Digital is solving the documentation piece. We solve the scheduling piece. Neither problem is the whole answer. But if you are still writing your schedule by hand or if your intake coordinator is still re-typing referral data from fax PDFs, you are carrying costs that show up in your margins, your turnover, and eventually your star ratings.
CMS has been transparent about the link between staffing consistency and HHVBP quality scores. Consistent staffing requires consistent scheduling. Consistent scheduling requires a system built for the actual complexity of the problem.
What I know for sure
Nurses are natural innovators. We sit at the bedside, and we see the problems. We may not always think of ourselves that way, but we are. The scheduling problem my husband solved for me was not something I went looking for. It was handed to me as an additional duty and it was awful, and eventually, someone who loved me got sick of watching me suffer through it.
That is a lot of how healthcare innovation works. Someone gets close enough to the pain to actually feel it, and then they build something.
The tools we have now make that faster and more powerful than at any previous point. But the tools only work if the people using them understand what problem they are actually solving, and can evaluate whether the output is getting them there.
I got back on the floor because an algorithm took 18 hours of schedule writing and turned it into five minutes. My nurses got a fairer schedule, and they knew it. Nobody was accusing me of being a favorite anymore.
That is what this is supposed to feel like.
Frequently Asked Questions
What is combinatorial optimization in nurse scheduling?
Combinatorial optimization is a type of algorithm that evaluates a very large number of possible schedule configurations and identifies the one that best satisfies all constraints, certifications, shift patterns, coverage requirements, staff preferences, and more. Unlike rules-based scheduling software, it does not just check whether a schedule is valid. It finds the best possible valid schedule from billions of options in minutes.
How is AI nurse scheduling different from traditional scheduling software?
Traditional scheduling software helps you build and display a schedule. AI optimization actually generates the schedule by evaluating constraints at a scale humans cannot match manually. The difference is between a tool that organizes your work and one that does the computational work for you.
Why does nurse scheduling affect patient care quality?
Scheduling affects nurse fatigue, continuity of care, and staffing consistency, all of which are tied to patient outcomes. CMS quality measures under HHVBP include metrics sensitive to staffing consistency. Agencies with unstable or inequitable scheduling tend to have higher turnover, which directly disrupts patient-clinician continuity.
Can AI scheduling work for home health agencies specifically?
Yes, though it requires configuration for the specific constraints of home health: geographic routing, certification matching by patient need, visit type requirements, and clinician availability windows. The underlying optimization problem is well-suited to algorithmic scheduling; the complexity is, if anything, higher than hospital floor scheduling because of the routing dimension.
What is the connection between nurse scheduling and clinician burnout?
Scheduling inequity, where some nurses consistently receive worse shift patterns than others, is a documented driver of burnout and turnover. A 2025 study in JMIR Formative Research found that nurses in both hospital and home care settings reported that perceived unfairness in scheduling reduced job satisfaction and contributed to intent to leave. Algorithmic scheduling that is transparent and preference-aware directly addresses this.

