Blog
Mar 30, 2026
Home Health Is Not What Most People Think It Is

Kathy Duckett

I started my career carrying a bag in Detroit. I knocked on doors in neighborhoods I did not grow up in, walked into homes where people were figuring out which medications they could afford that month, and sat with patients who were trying to recover from surgery in whatever space and with whatever support they had available. That experience taught me something that still guides everything I do: regardless of circumstance, sick people want the same thing – they want to not go back to the hospital again. And my job, then and now, is to help them get back to the level of independence that is possible for them.
More than 30 years later, I am doing the most interesting work of my career. I joined Copper Digital as a clinical advisor to help shape AI tools for home health documentation. When Arvind asked me to join the Inside Home Health podcast and talk about why home health matters, I realized how much confusion still exists, even among people who work adjacent to the industry, about what home health actually is, what it is designed to do, and why getting the documentation right is so consequential.
I want to clear some of that up. And then I want to explain why, after 30 years, I believe we are finally at the point where technology can genuinely help.
Home Health Was Designed as a Bridge, Not a Destination
When Medicare was created in the 1960s, home health was built into the program as a specific type of benefit with a specific purpose. The idea was straightforward: after a hospitalization, patients needed a bridge between being completely cared for in a hospital and being fully independent at home. Home health was that bridge.
That design intention has not changed. Home health is intermittent, short-term, and episodic. The expectation is that you will need it for a finite, predictable period, generally 30 to 60 days, though we do recertify patients who need more time. The goal when I walk through a patient's door is never to take over their care indefinitely. It is to figure out, from the moment I arrive, when and how we are going to help this person stop needing us.
That is the mandate. Get you to independence, or get you the resources that make independence possible, whether that means outpatient therapy after a hip replacement, hospice when the clinical picture changes, or a different care setting if the home environment cannot safely support recovery.
When we walk in the door, we have to figure out when we are going to stop taking care of you. That is not a limitation. That is the design. |
Home Health vs. Home Care
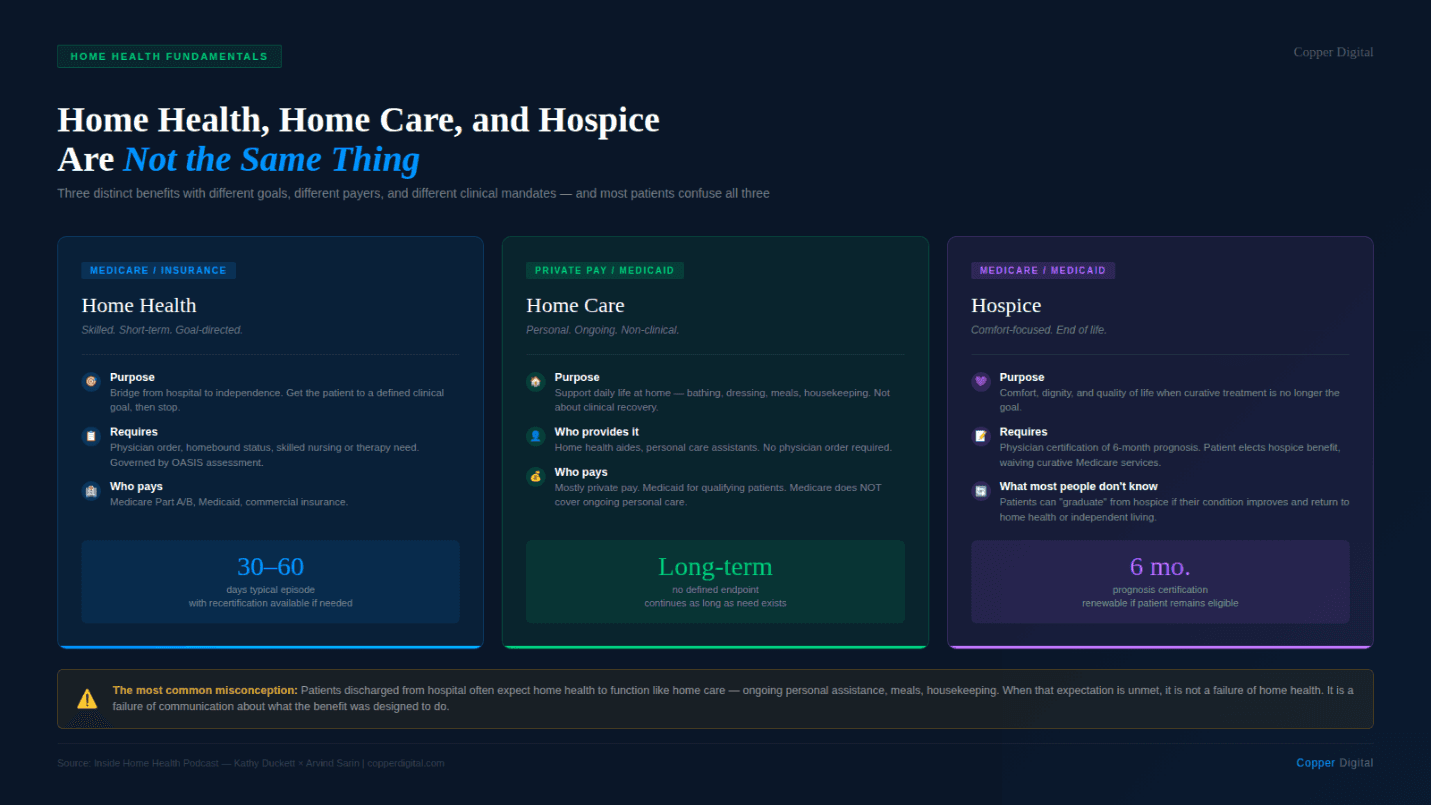
This is the distinction I spend the most time clarifying, including with people who have been working in and around this industry for years. Home health and home care are not the same thing, and the confusion between them creates real problems for patients, families, and agencies.
Home health, as paid by Medicare and most insurance, is a skilled care benefit. It requires a physician's order. It is generally tied to a homebound status determination. It is clinically driven. Usually it is a registered nurse that comes in and does a full assessment. . Occaisionally there is no need for registered nursing care, only therapy. It that case, a Physical Therapist with come in and do the initial full assessment. The plan of care is based on what the patient needs to reach a defined clinical goal. It is not open-ended.
Home care is something different. It refers to personal care support, help with bathing, dressing, meal preparation, and housekeeping. It can also be used to provide shift-level nursing care. But the key is that it is not a skilled benefit under Medicare. Most of it is paid privately or through Medicaid, depending on the state and the patient's financial situation. It is often long-term because the need it addresses is not episodic.
The confusion matters because patients frequently come home from the hospital expecting home health to do both. They think someone is coming to take care of them. They want to show us the spare bedroom. And when we explain that our job is to help them become independent, not to provide ongoing nursing or personal care, it can feel like a disappointment. Families who are counting on support they thought was covered find out it is not. That is a real problem, and it starts with a fundamental misunderstanding of what the benefit was designed to do.
Hospice Is Also Misunderstood, Including the Part About Graduating
Another distinction worth drawing clearly: hospice is its own benefit, and it operates on completely different terms than home health.
Hospice care is for patients at the end of life, with a prognosis of six months or less if the disease follows its expected course. The focus shifts from curative or restorative goals to comfort and quality of life. It is a different clinical model, different staffing, and a different reimbursement structure.
What most people do not know is that hospice is not always a one-way door. Prognosis is medicine's best estimate, not a guarantee. I have had patients placed on hospice who, six months later, were doing significantly better. In those cases, they can graduate from the hospice benefit. We stop the hospice service because the clinical picture no longer supports it. They can then transition back to home health or to independent living, depending on where they are.
I ran a hospice alongside a home health agency f and saw this happen more than once. The benefit is written the way it is because we have to work within the parameters of how Medicare defines these services. But the clinical reality is more nuanced than the benefit structure suggests, and patients and families deserve to understand that.
Why People Recover Faster at Home
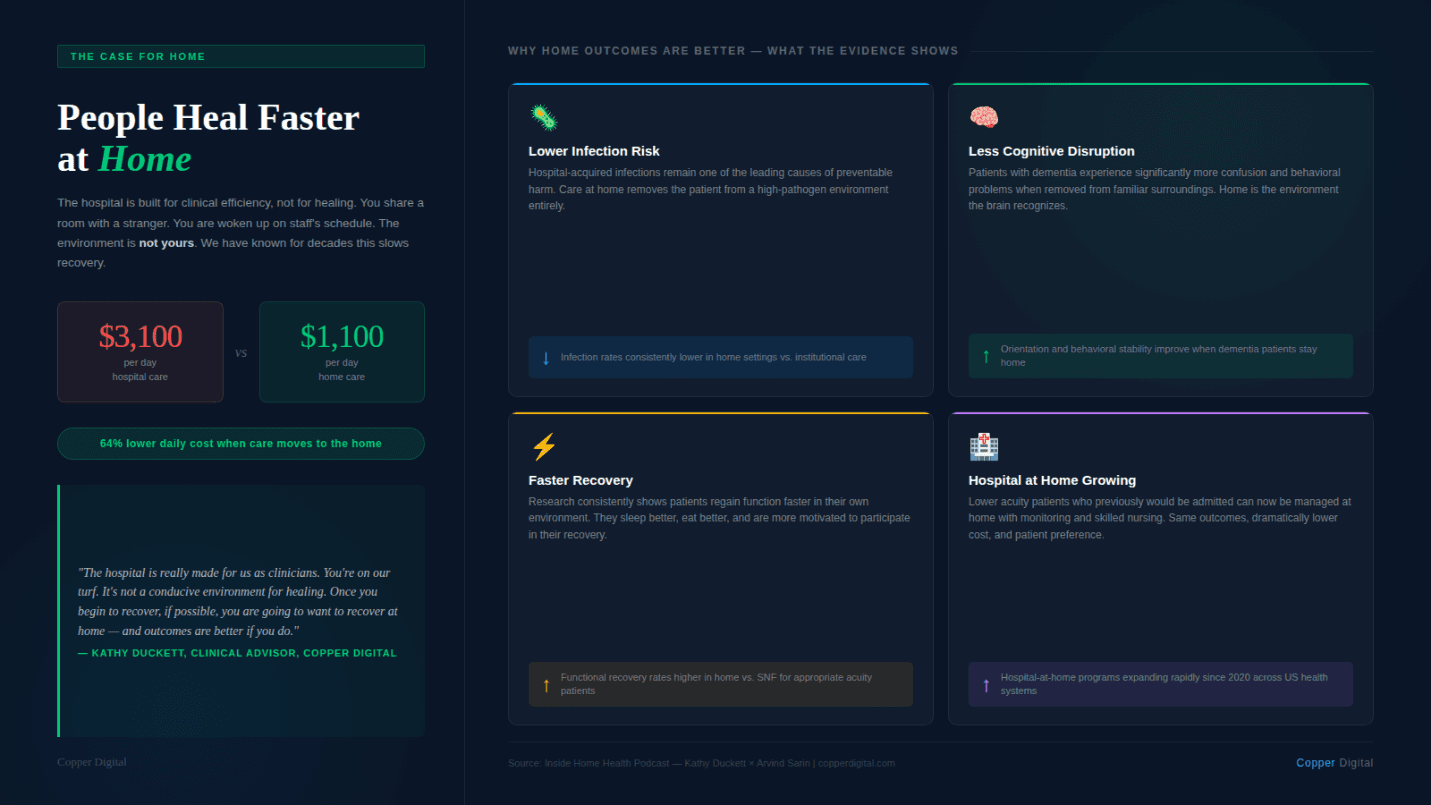
There is solid evidence behind the push to move care out of hospitals and into home settings. Patients heal faster in their own environment. Infection rates are significantly lower at home than in institutional settings. Patients with dementia experience considerably less confusion and behavioral disruption when they are cared for in a familiar environment rather than displaced to a hospital.
The hospital is a clinical environment built for clinical efficiency and to treat acute health care issues. You are awakened when the staff needs to check on you. Tests happen on the hospital's schedule. You share a room with a stranger. The bed is not comfortable. None of that is conducive to healing, and we have known that for a long time.
That is the logic behind hospital-at-home, a model that has been growing rapidly. For patients with lower acuity diagnoses who have the right support structure, managing their acute episode and recovery at home, with appropriate monitoring and skilled nursing visits, produces better outcomes at lower cost. The numbers Arvind shared in our conversation reflect what the research consistently shows: a hospital day costs roughly $3,100. A day of care at home costs roughly $1,100. That difference, compounded across the population, is significant.
People get better faster when they are in their own home. We know that. Infection rates drop. Outcomes improve. The challenge is figuring out how to deliver that care effectively with the workforce we have. |
The Workforce Problem Is Real, and It Changes Everything
Home health is capacity-constrained in a way that hospital care is not. In a hospital, you have teams of clinicians available on site. You have backup. You have colleagues in the next room. In home health, a nurse goes into a patient's home alone. She cannot see more than one patient at a time. Her daily capacity is limited by driving time, assessment complexity, and documentation burden.
We do not have enough nurses. That is not a new statement, but it is an increasingly urgent one. And the way we are currently asking those nurses to spend their time, including the hours they spend on documentation after the visit, is a significant part of why we cannot retain the ones we have.
If we are serious about shifting care to the home, we have to figure out how to make home health nursing sustainable. That means reducing the documentation burden without sacrificing accuracy. It means building tools that work with clinical workflows instead of against them. And it means understanding that every hour a nurse spends reconstructing visit notes from memory is an hour of clinical risk, not just an HR cost. I covered this in more depth in Your EMR Was Not Built for Your Nurses.
OASIS Is Central to Everything, and Most People Do Not Know It Exists
For anyone outside the industry, OASIS stands for Outcome and Assessment Information Set. It is the standardized assessment instrument that Medicare-certified home health agencies use at the start of care, at key time points during a care episode, and at discharge. It has been part of the Medicare home health program since the late 1990s and has gone through several iterations, most recently OASIS-E and the upcoming OASIS-E2 changes.
The OASIS is not just a form. It is the foundation of almost everything that matters in home health. The answers to those questions determine the patient's reimbursement under PDGM. They feed into the agency's quality measures and star ratings on the CMS Care Compare site. They establish the baseline from which outcomes are measured. They inform the plan of care. And they are subject to audit.
What I tell clinicians when I am training them is that accurate OASIS coding is both a clinical and a financial imperative, and those two things are not in conflict. Coding accurately is coding honestly. It is describing what you actually found when you walked in. The goal is not to code the patient as sick as possible to maximize reimbursement. It is not to code them as healthy as possible to look good on outcomes. It is to document what you actually observed, using the specific parameters that CMS has defined for each question.
Why nurses get it wrong more often by mistake rather than getting it wrong on purpose
In my experience, the vast majority of OASIS inaccuracies are not fraud. There are errors. Nurses are working from memory hours after a visit. They are rushing through 150 or more questions after a complex two-hour assessment. They answer one section without realizing it contradicts something they entered three screens earlier. The EMR does not catch it. Nobody catches it until QA or, worse, an auditor.
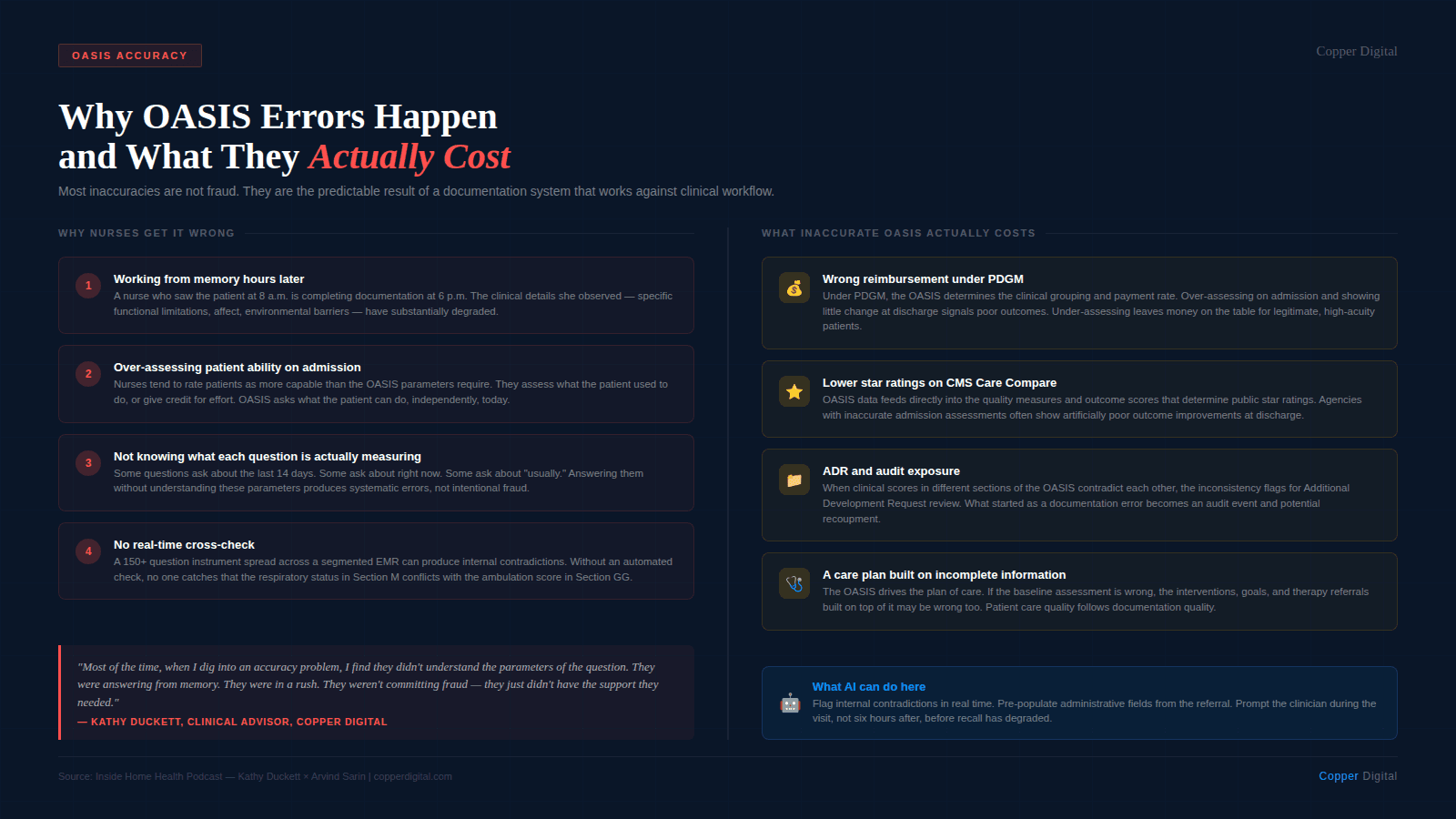
The other thing I consistently see is that nurses tend to over-assess patient ability on admission. They see the patient at their best, or they give the patient credit for what they used to be able to do, rather than what they can actually do today. Or they see what the patient is doing, but not doing safely, and they forget that the OASIS question asks “can the patient do this safely?”. That creates a documentation problem at discharge: if the patient looked functional on admission, demonstrating meaningful improvement becomes very difficult. I covered this dynamic in detail as part of my conversation with Gaurav Henry, which became the blog post Why Your Clinical Story Does Not Make Sense.
The challenge is not that nurses want to commit fraud. The challenge is that they do not understand the specific parameters of each OASIS question, or they are answering from memory at six in the evening about a patient they saw at eight in the morning. |
Where AI Can Actually Help
I want to be precise about this because I have seen the field get carried away with what AI promises to do. AI is not going to replace clinical judgment. It cannot observe a patient. It cannot read the room. It cannot pick up the subtle signs that something has changed between the last visit note and what is happening right now in the patient's living room.
What AI can do, and what I believe Copper Digital is working toward in a way that takes the clinical reality seriously, is handle the pieces of documentation that do not require clinical judgment. There is a significant amount of information that comes into a home health agency on a referral that never makes it efficiently into the OASIS workflow. A 30-page hospital discharge packet gets faxed over. The nurse does not have time to read it before walking in. So she walks in without the context she needs.
AI can extract the relevant clinical nuggets from that referral. It can synthesize what matters for this visit. It can pre-populate the administrative fields that do not require assessment. It can flag contradictions between sections of the OASIS before they become an audit finding. And it can prompt the nurse when something appears to be missing, during the visit, not hours after.
The pre-visit briefing Arvind and I discussed is a good example of what this looks like in practice. Before walking in, the nurse should receive a short paragraph: here is what happened on the last visit, here is what the plan was for today, and here is what has changed since the last nursing contact, including labs, physician visits, and therapy notes. AI can produce that. That is not replacing the nurse. That is giving her the information she needs to walk in prepared rather than having to reconstruct context from a cold chart. This connects directly to what we described in An Autopsy of a Start of Care: The 2-Hour Visit That Takes 6 Hours.
Why I Joined Copper Digital
I have spent my career at the intersection of clinical practice and technology. I was an early advocate for remote patient monitoring. I helped agencies build telemedicine programs before telemedicine was mainstream. I have seen a lot of technology promise to fix home health documentation, and I have seen most of it make the problem worse by adding complexity without clinical understanding.
What drew me to Copper Digital is that Arvind is asking the right question. Not what can AI do, but what does the nurse actually need in the patient's home, and how do we build around that reality rather than asking her to adapt her workflow to fit a tool?
I am two weeks in as a clinical advisor, and my job is to make sure that clinical empathy is built into the product design from the beginning. Not added later. Not treated as a compliance checkbox. Built in from the start, because that is the only way the technology is actually going to work for the people who need it most: the nurses in the field, the patients recovering at home, and the agencies trying to survive and grow in an environment that keeps getting harder.
Home health deserves better technology. It has been underinvested in for decades, partly because it is not glamorous, partly because the regulatory environment is complex, and partly because the people closest to the problem, the field nurses, are never the ones in the room when the product decisions get made.
That is what I am here to help change.
Listen to the full conversation with Arvind Sarin on the Inside Home Health podcast series at copperdigital.com/blog/inside-home-health. To see how Copper Digital is building AI agents that support home health documentation and OASIS accuracy, request a demo. |
About the Author
Kathy Duckett is a nationally recognized leader in home health and hospice operations, clinical practice, and healthcare technology strategy. She has spent over 30 years working at the intersection of nursing practice and technology, serving in roles ranging from field nurse to Director of Advanced Care at Home to Chief Clinical Officer . She joined Copper Digital as a Clinical Advisor in 2026 and serves as a voice for clinician-centered product design.
Related Reading

